Experts on Vexing Vaccination Challenges and Beating the Pandemic
February 25, 2021
- Author
- Jay Pfeifer
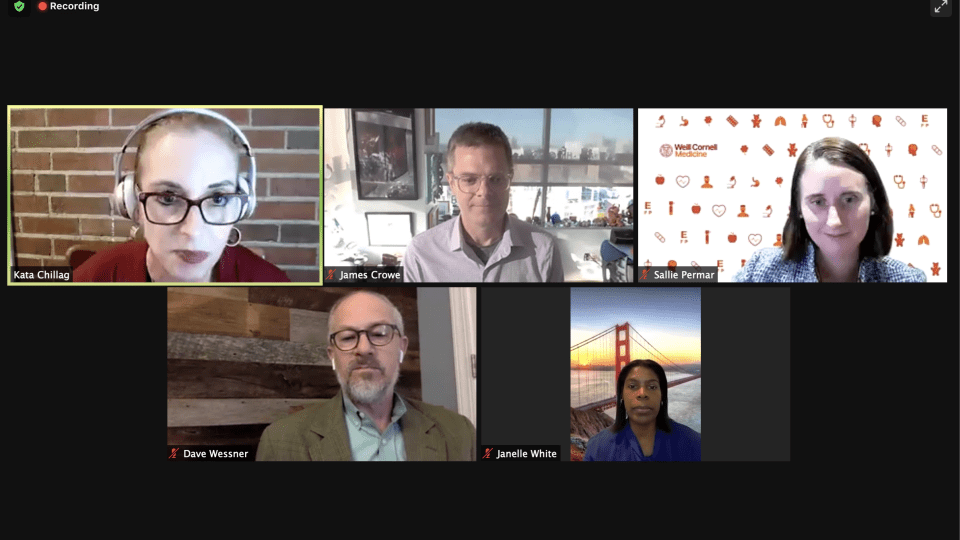
Kata Chillag, Hamilton McKay Professor in Biosciences and Human Health, Davidson College; Janelle White, M.D., Medical Director of Community Health, Atrium Health; Sallie Permar ’97, M.D., Chair of the Department of Pediatrics, Weill Cornell Medicine; James Crowe ’83, Director of the Vanderbilt Vaccine Center, Vanderbilt University; Dave Wessner, Professor of Biology, Davidson College
The casualties of the pandemic extend beyond the half-million tragic deaths and millions of COVID cases.
Davidson College convened a group of experts across disciplines to discuss the U.S. COVID-19 vaccine rollout and answer questions about the safety and efficacy of the new drugs that offer hope for a way out of the pandemic.
Large swaths of the public have lost trust in medicine, government, science and each other.
The recent dashboard numbers are encouraging. Vaccinations are up. Cases are down. But five experts in public health and immunology gathered by Davidson College and Atrium Health this week offered not a “Doom Zoom,” but a wider and longer view of the country’s vaccination situation, including a slew of accompanying and unmet challenges.
They pointed to damage beyond the terrible human toll. The pandemic exacerbated inequality, mainstreamed misinformation and spotlighted the struggle of adapting to a challenge about which we know very little, said Kata Chillag, chair of Davidson’s new public health academic department and the event’s moderator.
Janelle White, M.D., a panelist and a pediatrician and medical director of community health for Atrium, often is asked whether COVID vaccines can be trusted.
“That’s something I hear a lot,” said White, “particularly in our marginalized, underrepresented minority communities.”
The speed of vaccine development is a marvel to some, and a source of concern for others.
“The process has been fast,” said Dave Wessner, biology professor at Davidson, “but I don't think it’s been rushed. Those are two different things.”
The time from discovery to vaccine was “the fastest in history,” said James Crowe, director of the Vanderbilt Vaccine Center and a 1983 graduate of Davidson.
The question he hears is: What shortcuts were taken?
“And the answer to that is there were no shortcuts,” he said. “The time was compressed. But all of the same stuff was done as would normally be done. And you can measure that by how much money was spent. You can spend the same amount of money over 10 years, or you can spend it all in four months, but the actual steps that would normally be taken were all taken.”
The vaccine technology draws questions and skepticism because it sounds new, panelists said. The vaccines use mRNA, genetic material that delivers instructions for the body to make proteins.
“It actually was not that new,” said Sallie Permar, Davidson class of 1997 and chair of the department of pediatrics at Weill Cornell Medicine. “For at least a decade or so, the mRNA technology has been tested for things like cancer therapy. This was not a brand new technology, but the timing was exactly right. Enough development had gone on with the mRNA platform that it was ready.”
Critical Threshold
Permar estimates that 80 percent of the population will need to be immune to the virus that causes COVID-19 for herd immunity to take effect.
Distrust in the vaccine makes reaching that crucial threshold very difficult.
National polls show 30 to 40 percent of Americans unwilling to get a COVID vaccine. A North Carolina poll in December showed 20 percent unwilling and another 40 percent reluctant.
“If we have a situation where 50 percent of the people for whatever reason are reluctant to get to the vaccine,” Wessner said, “we’re never getting to that herd immunity status.”
A continuing threat to vaccine adoption is social media, where falsehoods spread as fast as the virus.
“Does mRNA sterilize you? No,” said Crowe, reciting from the stream of online conspiracy theories. “Are there little chips in these things? No, there are not. Does this modify your DNA? No possible way. These kind of crazy ideas are gripping the minds of millions, maybe tens of millions or hundreds of millions of people. And there’s no basis in fact.”
The COVID-19 threat will fade, Crowe said. And decisions are needed now—while the memory is fresh—about how the nation will prepare for the next pandemic. Because there will be another.
“We already know the sequences of coronaviruses that could do the exact same thing, again,” he said. “We know that right now, today. And the question is: Do we have the political will as a people to tell our legislators: We want to invest our tax dollars and effort in looking forward, rather than saying, ‘I hope this all goes away.’”
The virus data seem to be improving, but all five experts agreed that the public health mitigation strategies in place—social distancing, masks, hand-washing—are still essential.
No one should see a vaccine as a magic bullet that eliminates the need for prevention and safety measures, White said: “We don’t want there to be the thought that we can take our foot off the gas.”